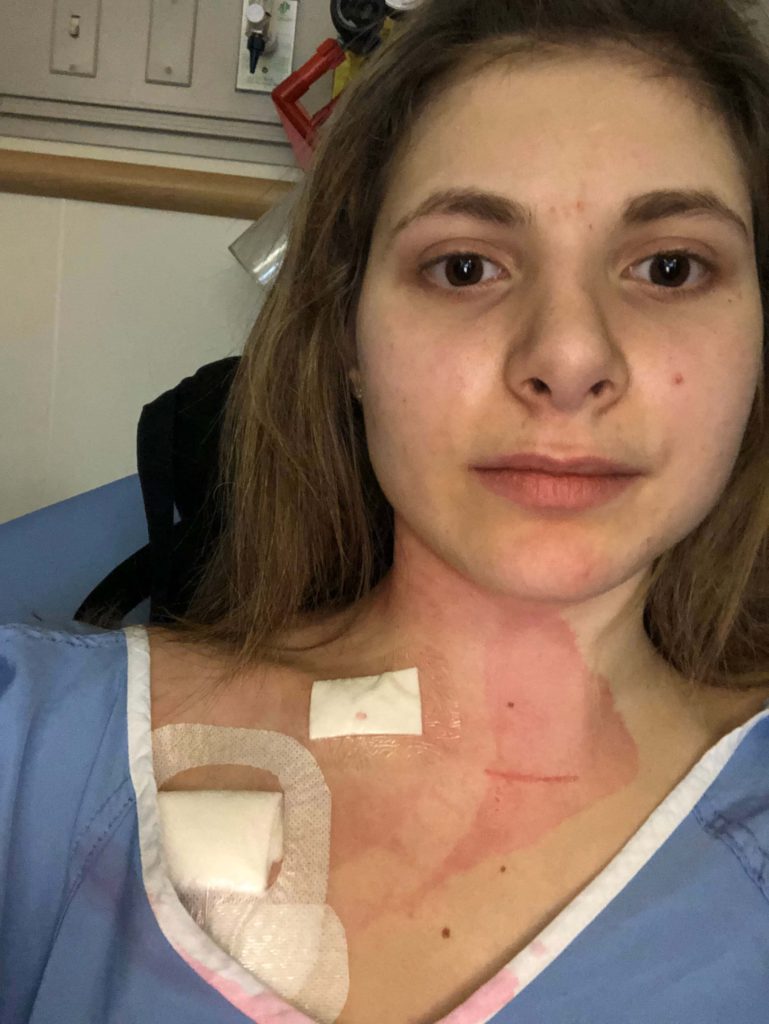
Ava’s Stage 4B Classical Hodgkin’s Lymphoma Story
1st Symptoms: Trouble digesting, weak immune system, raised glands, night sweats, chest pain, extreme fatigue
Treatment: 6 cycles of ABVD chemotherapy
Topics: Emotional grieving, mental health, letting go
Ava’s Stage 4B Classical Hodgkin’s Lymphoma Story
Ava shares her in-depth stage 4B Hodgkin’s lymphoma story, from getting diagnosed to undergoing ABVD chemotherapy. Ava also highlights dealing with survivorship and finding a cancer community.
- Name: Ava O.
- Age when diagnosed: 21
- Diagnosis:
- Hodgkin’s lymphoma
- Stage 4B
- 1st Symptoms:
- Trouble digesting
- Weak immune system (always sick)
- Raised glands
- Night sweats
- Chest pain
- Extreme fatigue
- Extreme pain in shoulder blade and abdomen
- Tests & Biopsies:
- Chest CT scan & X-ray
- Echocardiogram
- Biopsy of gland
- PET scans
- Blood work before every treatment
- Treatment:
- ABVD chemotherapy regimen
- 6 cycles
- Each cycle = 1 month, biweekly
- Total: 12 infusions
- 6 cycles
- ABVD chemotherapy regimen
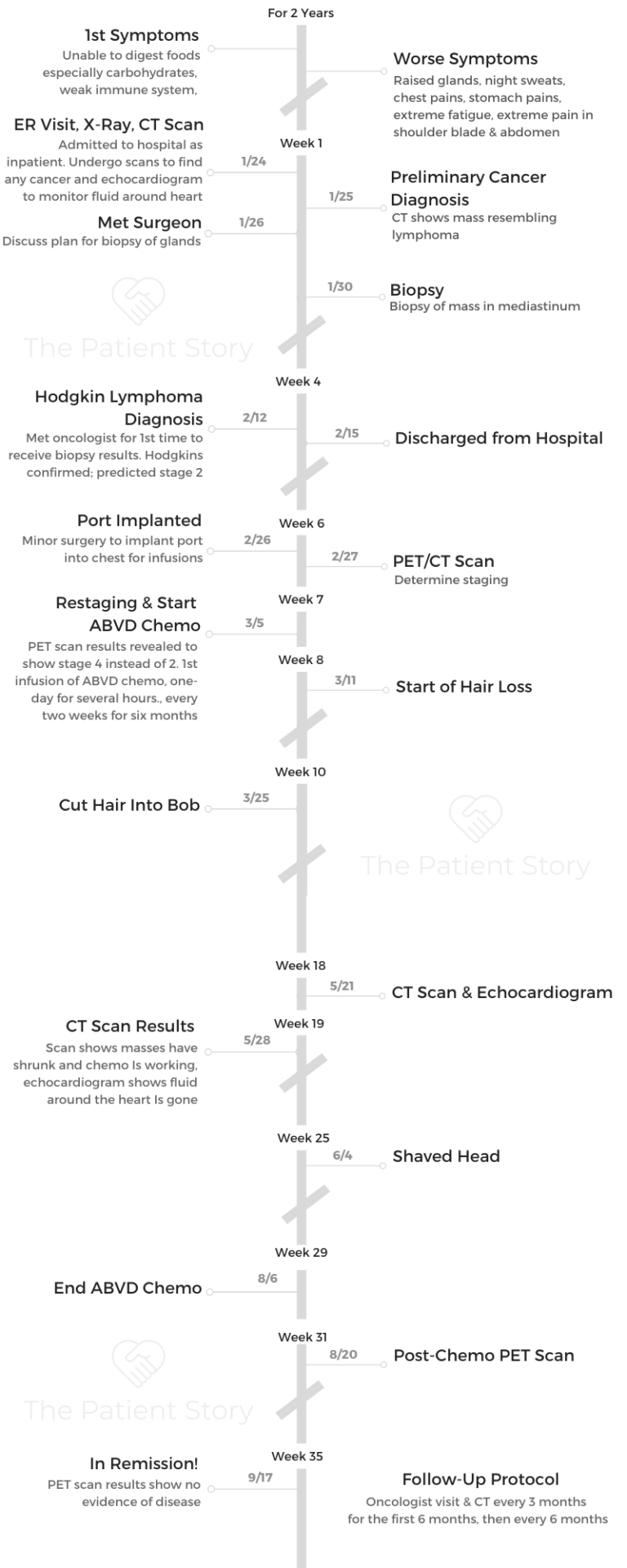
- First Symptoms
- How old were you when you were diagnosed?
- How did you know something was wrong?
- Describe how the symptoms got worse
- It was tough to put all the symptoms together
- You discovered you had exhibited "rarer" lymphoma symptoms
- Noticing other behavior changes
- Doctors never suspected cancer
- Despite missing the cancer, you feel doctors did the best they could
- Cancer hid behind other medical issues
- Diagnosis
- Preparing for Treatment
- ABVD Chemotherapy
- Hair Loss After Chemo
- Scans and Treatment Progress
- Reflections
This interview has been edited for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
Unfortunately, I think many cancer patients would agree that you tend to go to a ‘nothing place.’ You’re there, but you’re not there. Someone could tell you something, and you go, ‘Oh, okay,’ and nod your head.
Running took me there when I wanted to, and it helped me not taste chemicals. I would forget about the chemicals and how tired I was. It was just me and the road.
Ava O.

First Symptoms
How old were you when you were diagnosed?
I was diagnosed with Hodgkin lymphoma less than a month after my 21st birthday.
How did you know something was wrong?
I knew something was wrong about a year and a half before I was diagnosed because I couldn’t digest carbohydrates properly without any given reason, and I was always getting sick. Other than undergoing corrective spine surgery when I was 15, my medical history was perfectly clean.
In January, I came down with something. It made me feel very weak, extremely nauseous, and I lost about 10 pounds during it. I had vertigo and coughed relentlessly for months.
At first, doctors in the ER questioned if I had something like whooping cough, but after several test results that showed that I was healthy, it appeared that I simply had a bad strain of the flu.
I totally lost my voice for about a month, and then after that, my voice would come and go. I noticed it would disappear when I drank alcohol or consumed foods containing lots of sugar and carbohydrates. I was rather athletic, but all of my muscles seemed to disappear at the same time.
To top it off, the amount that I was coughing actually led me to fracturing my ribs more than once. I missed so much class time because of how sick I was and ended up having to drop my classes halfway through my semester.
From that point onward, the coughing came and went, but never totally went away. I became more and more prone to catching colds very easily.
By mid-2017, I was constantly getting sick. Every time I recovered from a cold, I would catch another one, and again, the coughing lasted for months. As time passed, my glands under my jaw began to feel inflamed.
If my friends were sick, they knew to stay away from me because of how much a cold would actually impede my ability to function. My weight dropped by nearly 8 pounds and then slowly fluctuated back to normal. My body’s response to consuming sugar and carbohydrates became worse. They would made me feel drunk. I know that sounds totally crazy.
I tried to discredit that possibility so many times, but it is the truth. The day after consuming alcohol/sugar/carbs, including the healthy ones, I would feel hungover, and the glands under my jaw would be totally swollen.
Other than having a slightly abnormal white blood cell count, my medical tests showed that I was healthy, even though I didn’t feel healthy.
I saw a naturopath, who suggested we cut carbohydrates out of my diet and then reintroduce them later. I did what I could to maintain my quality of life, which meant trying it out. It wasn’t something I wanted to do since carbs are pretty important to your health, but my body wasn’t tolerating them. It was getting in the way of my ability to function.
In the end, I did what I had to do, thinking that everyone has something to deal with and that I was lucky that my health was still intact. It worked well, and my pains and discomfort diminished significantly until we tried to reintroduce the carbs. When we did, my body went into a frenzy of all of the symptoms I’ve mentioned, only they came back much worse.
All in all, my first symptoms were the swollen glands under my jaw, being unable to fully recover from a cold, facing adverse responses to alcohol and carbohydrates, and experiencing ongoing thrush/yeast infections.
Describe how the symptoms got worse
At the beginning of the next year, I felt my first raised gland in another area of my body: the inguinal area, which is below your pelvis. I mentioned it to my doctor, but it was believed not to be of significance, just as the glands under my jaw were believed a result of something harmless.
Then I faced excruciating pain in the left side of my chest that lasted for a couple of weeks. I couldn’t get out of bed without help.
It was thought to be a result of my scoliosis, although I had never felt shooting pain there before.
I experienced major stomach spasms in July 2018 that were inconclusive. Soon after, I faced an unforgiving nerve pain in my left shoulder blade, which was attributed to scoliosis.
The glands under my jaw were still deemed as harmless, and then they made an appearance near collar bones. Those largened over time. I also began to feel warmer than usual, and by August, I had night sweats.
I had been to see my doctor so many times, had a few trips to the ER, and underwent so many tests, all of which showed that I was still healthy. As time passed, the nerve pains in my left shoulder blade continued and spread to new areas of my body. My diet became more restrictive as my body’s ability to tolerate food decreased.
My strict diet continued, and changing it caused my body to go absolutely haywire. I was eating basic vegetables and getting nutrients from highly (healthy) fatty foods and protein to maintain my weight.
I was constantly calorie counting to make sure I was eating enough. I loved food, and I couldn’t eat even half of the food I loved. I was eating so much of the same foods, and I was eating constantly. I would eat a lot of avocados, almonds, chicken and eggs regularly as meals, and I also ate them in between meals.
Other normal foods (like potatoes, fruit, eggplant, toast, yogurt, carrots) would have the same effect on me as they did the year before, only worse. I would be flat on my back for weeks in pain.
My weight dropped again in December, and my muscle disappeared with it, without returning even as my weight restored itself. I was then forced to blend the basic foods I could eat if I were to eat without throwing up, enduring agonizing pain that was not diagnosed beyond IBS, or facing blood in my stool.
Between November 2018 and January 2019, I had been taken and wheeled to the ER 4 or 5 times because of how much unexplained pain I was in. I would plead to the doctors, begging them to believe that I had an extremely high pain tolerance and that I was truly in so much pain.
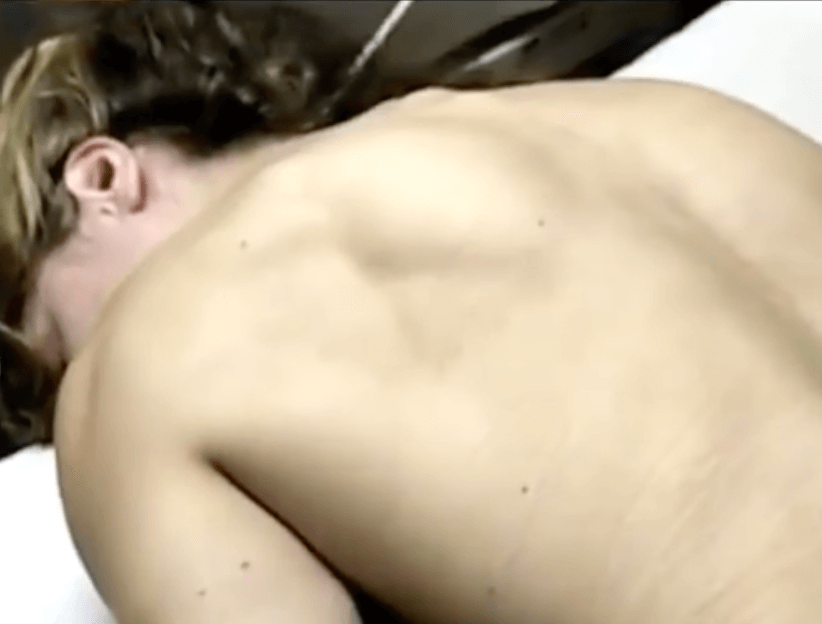
It was tough to put all the symptoms together
My key symptoms happened slowly and one at a time, almost making it appear as though they were all unrelated. My stomach pains, attributed to IBS (irritable bowel syndrome), occurred in the upper left quadrant of my abdomen, where the spleen is located.
Upon my diagnosis, I learned that having an enlarged spleen is a symptom of lymphoma, and it was causing my pain. The relentless nerve pain I experienced in my left shoulder blade, attributed to scoliosis, was parallel to the location of the mass growing in my chest.
Looking back, I was also actually quite itchy for some time, but I only realized that itchiness is a symptom of lymphoma much later.
There wasn’t one specific “classic” symptom that I identified with. I identified with many of them, as they occurred simultaneously. My downfall was a slow progression. It didn’t just happen in one day. It took many months and over a year for my symptoms to cause visible changes of concern.
You discovered you had exhibited “rarer” lymphoma symptoms
I couldn’t drink alcohol without the lymph nodes under my jaw becoming inflamed and painful. My doctor and I thought I was just sensitive to alcohol.
After my diagnosis, I learned that my body’s response was actually a rarer symptom of Hodgkin Lymphoma.
Noticing other behavior changes
I never nap, and I have never needed to nap to maintain functionality during the day, but in September (2018), I started to need to nap in order to have the energy to get things done. I went to sleep at 10 p.m., woke up at 8 am, and after having 10 hours to sleep, I still felt drained.
I began to think that being in pain was my new permanent normal. Coping was my new normal, well before my diagnosis actually happened.
Doctors never suspected cancer
They couldn’t find anything specific for a while (at the doctor’s office). It was masked behind IBS symptoms and residual scoliosis pains. Cancer exists at a cellular level before it manifests as masses.
The only medical test that showed signs of abnormality were my blood test results, which consistently showed that my white blood cell counts were slightly abnormal.
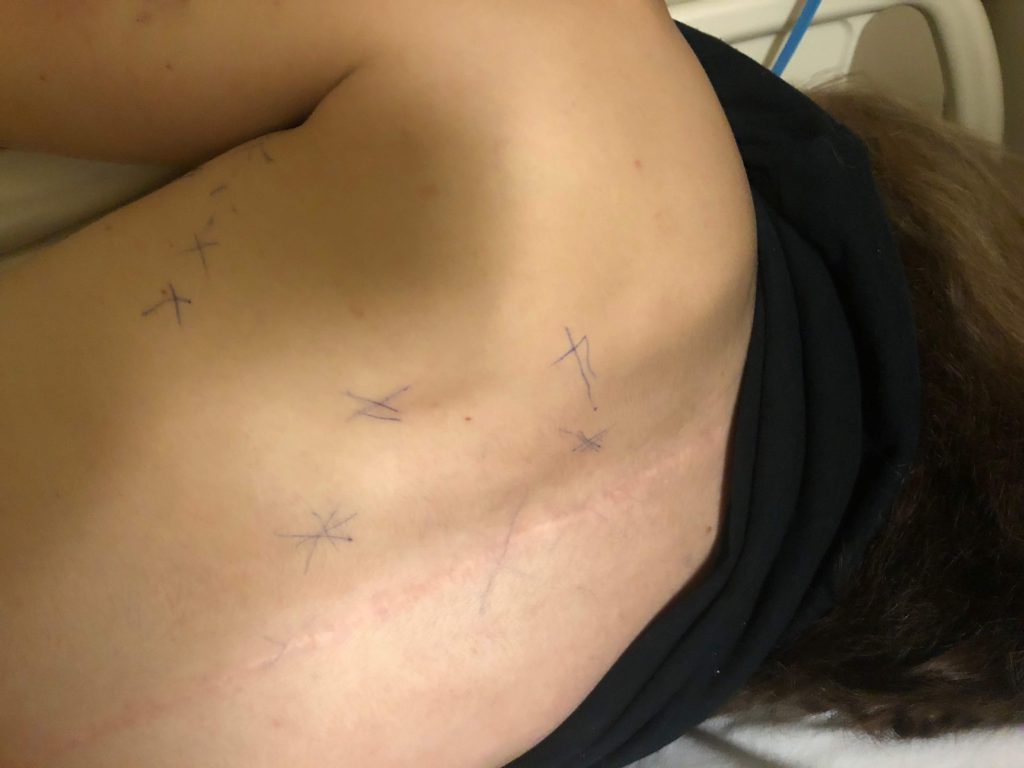
I started to take birth control in January 2018. At that time, my weight fluctuated up by about 8 pounds, but within a month of starting it, I lost all 12 pounds. I know when taking birth control, water weight increases. In my experience, the weight gained from birth control never dropped while I took it, so even if I lost some of the weight as my body learned to regulate on it, I likely shouldn’t have lost all of the weight. For the next several months, my weight fluctuated up and down by about 10 to 12 pounds.
During mid-2018, I felt so rundown, and the length of my list of symptoms extended since they started. When I explained all of my symptoms to my doctor, she recommended I take a depression test, acknowledging that my medical records showed that I faced a depressive episode several years earlier.
At the time, I was recovering from an 8-hour-long corrective spine surgery that involved implanting 2 foot-long rods into my spine and a double spinal fusion. The rods needed to be left alone to heal, and any physical jarring would have caused serious damage, so I had to stay home for months.
I was 15, and I couldn’t do anything I loved until I was fully recovered, which meant recovering for 2 years until I was 17. I endured a lot pain during that time, after all of the pain I endured before the surgery due to scoliosis. My depressive episode was the result of that.
Needless to say, I took the depression test, which I passed. I had never faced chronic depression, and overall, I had always been a happy person.
I felt totally undermined for being honest about how sick I was. I think her suggestion may have been more sensible if all of the physical symptoms I faced were not dismissed and a root cause was searched for until an answer was found.
I learned from my doctor’s response and approach to my yeast infections, which were not fully accounted for; my stomach pains, attributed to IBS; my worsening nerve pains, attributed to scoliosis; and my continuously fluctuating glands to believe that all of these symptoms were not to be concerned about beyond how they impeded my ability to carry out daily routines, to the point that I thought I was wasting ambulances when I needed them.
The only consistent sign that might have been telling were my consistently, slightly abnormal white blood cell counts. When one thing is consistently, slightly abnormal but everything else appears intact on paper, are you going to assume you have cancer? No. In fact, you’re told not to.
I had been seeing doctors all along since 2017. There didn’t seem to be a solution to all the pain that I felt under my jaw, in my stomach, in my chest and my back. That frustrated me. After several months spent tolerating such significant nerve pain, I finally could not bear it any longer.
My pain was the true catalyst behind why I ended up in the ER for the second time in less than 2 weeks on January 24th. It was the true reason behind my diagnosis. The ER doctors were concerned about the rods in my spine when I arrived.
Despite missing the cancer, you feel doctors did the best they could
You want to ensure that you’re being as fair as possible. My current GP met me when I was 18. Before then, I had a pediatrician who had known me all my life. Within a year of knowing my GP, my immune system was totally depleted, and I was getting sick all the time. In fairness, the Ava she saw at appointments was easily sick.
It didn’t seem abnormal for my white blood cell counts to be slightly raised considering how sick I’d get at different points. With that in mind, when you do the right things, you also have to take into account how long it occurs while you’re doing the right things and then figure out the reason behind why.
I go to a university in a different city than where my family lives. When I’d go to the ER when I was at university, I’d go to the ER there, and I would go to another one in Toronto when I was home.
Every doctor and nurse at St. Mary’s Hospital and Grand River Hospital in Waterloo was absolutely stellar. They were amazing doctors. Even without reason, since at different points in time nothing presented in my scans, they always looked deeper.
I don’t know how my scan from December 2018 led me to inconclusive results, and yet, within less than a month, the scan taken in January showed a mass in my chest.
Cancer hid behind other medical issues
Cancer hid behind an immune system that was perceived as weak, as well as symptoms that were chalked up as relating to IBS and scoliosis.
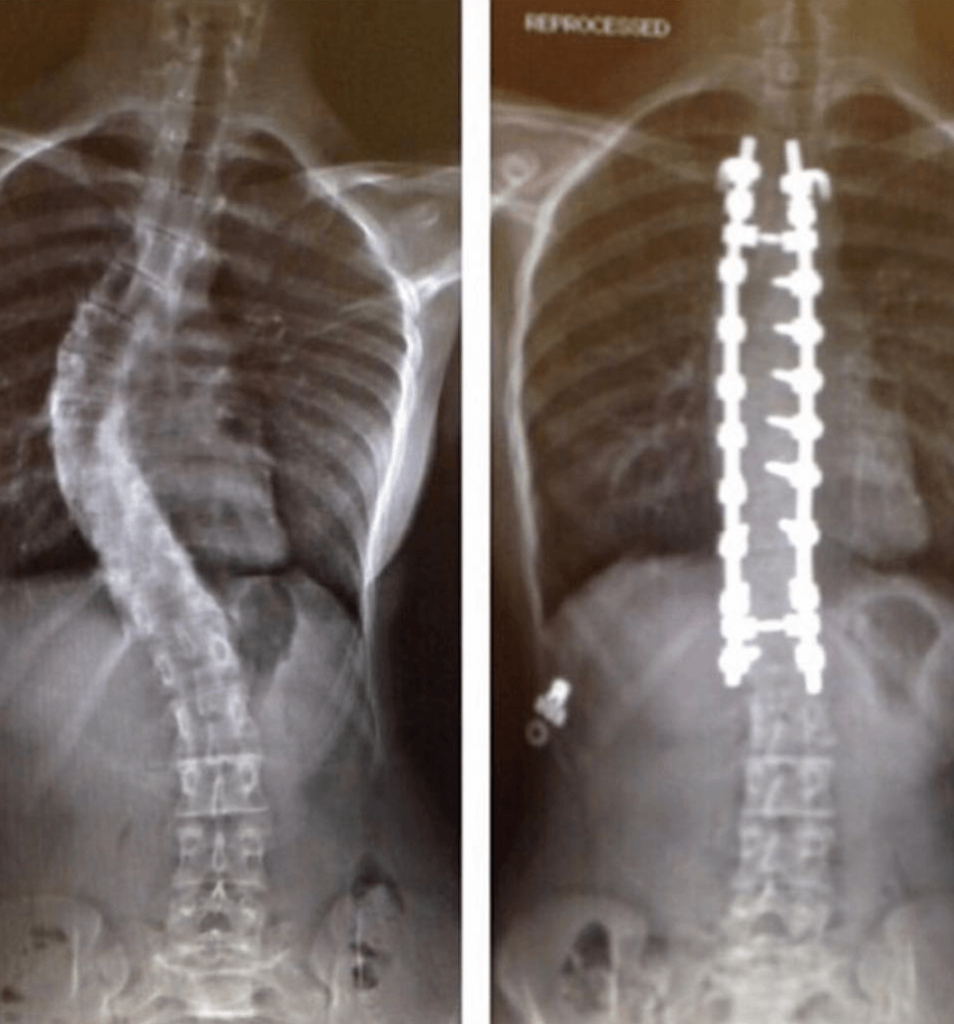
I also underwent spine surgery when I was 15 in 2013. Every now and again I go through nerve pain spams, which last for about a week. I’m talking about it in this interview as if it’s nothing, but I have just become so used to coping with the pain.
With that said, nerve pain is one of the top 3 most painful kind of pains that exists. When it’s there, there is no relief. It does not come in waves. It simply feels like your body is being pressed to a burning stove plate constantly. It’s just always there.
When this pain didn’t change after a week and then worsened for several other weeks and months, it was just a matter of time until breathing through it became useless.
Coping with pain was not new to me, and I was very good at it, but we all have a limit.
For me, it took years of unexplained symptoms, 6 months of constantly evolving pain, and 3 months of going to the gym to help my condition while it felt like my body was on fire until I couldn’t bear it anymore.
Diagnosis
What finally led to the discovery of cancer?
My back was in immense nerve pain that pain didn’t go away after a week, as it should have. It was present for months, worsened, and spread across my abdomen and down into my fingertips as time passed.
I was taken to the ER by ambulance in December a couple of times. On one occasion, I was huddled in a ball on the floor in my apartment in Waterloo.
I called my friend, who was about to hop on a bus to Toronto, at 7 a.m., sobbing because of the pain that rippled through my abdomen. He rushed over immediately and called 911. I remember crawling from my bedroom floor to the living room floor to unlock the door for him, remembering this pain from when I felt it back in July of 2018.
The other time I landed in the ER was when I was in Toronto. I was in the kitchen, and the nerve pain in my back was just relentless. I got on the floor in my kitchen and yelled for my mom. I was just lying there, screaming in pain.
I was a total mess, and my mom was just beside herself because she’d seen me in so much inconclusive pain for such a long. Every medical test had shown that I was perfectly healthy, and it just did not add up.
Both times I was in the ER that month, the doctors at both hospitals ordered scans, which both appeared as normal. The doctors administered morphine in an IV drip to relieve my pain (it didn’t work) and then sent me home.
On the day I was wheeled to the ER and later diagnosed, that severe nerve pain was still 100% present. The idea of breathing through the pain and talking yourself through it, saying to yourself, “It’ll be okay,” totally disappeared. I was at a point where that ability didn’t exist anymore.
Screaming in pain wasn’t embarrassing anymore. I just wanted it to stop. I begged and begged for an end to that pain. At that time, you could not touch my back in the area where I experience nerve pain because of how much pain it caused. It felt like stabbing to the touch. The ambulance paramedics had me hooked up to a morphine drip by the time I got to the hospital. It did nothing to relieve my pain, and I was in agony.
As soon as I arrived, doctors ordered several tests, but they had to try to get my pain under control so I could lie still for them. Doctors and nurses resorted to injecting fentanyl directly into my arms and legs to relieve my pain, and yet it was still ever-present. I just remember screaming, sobbing and begging for help.
I remember it as clear as day. The doctors and nurses said they had never seen anything like it before. Essentially, the meds calmed my body down, but it still felt like I was burning alive from the inside out.
They did their best to work quickly, and I did my best to lie still during my first X-ray scan. Then I had a few CT scans, an MRI. I was in the ER area for a while until I was told that I was being admitted.
The next morning, I woke up to a doctor’s voice. That was the turning point, marking the minutes when I went from being a 21-year-old girl to a 21-year-old patient.
The pain I endured had nothing to do with my previous spine surgery or IBS, and this time, the scans that were taken of my body did not come back clear. My health was not intact.

How did the doctor give the diagnosis?
She asked me, “Do you understand why you were been admitted?”
I remember saying, “Probably because I’m in so much pain that pushing fentanyl through my system has me loopy as hell, looking at you like you have 3 heads, and yet is not relieving my pain, but is making me tired enough to be still.”
I really did see 3 of her, and I really was still in so much pain. The medicine made me too drowsy to scream in pain, but it was there. Then she asked, “Where are your parents?”
I said, “They live in Toronto. I told them not to come up until today because every time I go to the hospital, I’m told I’m fine. I didn’t want to worry them at night over nothing. They’re on their way now. It’s actually comforting to know that this time, I wasn’t sent home.”
Then she said something that changed my demeanor. “It is best if we continue this conversation when your parents are here. I highly recommend that we wait until they arrive.”
I decided I didn’t want to wait if someone finally had an answer for me, so I called my parents and tapped speakerphone.
The doctor remarked that my X-ray scans showed what they called fullness in my chest, which led them to order a CT scan.
That showed a mass in my chest, resembling lymphoma. ‘Okay. What’s that?’ I asked.
She explained that lymphoma is a form of blood cancer. I actually remember feeling relieved to hear that. That sounds so absolutely strange, but I had been through so much trauma relating to my health for nearly 2 years.
By that point, I was very relieved to know it wasn’t in my head and there was finally an answer to all of my symptoms.
I remember saying, “Can we just talk about that after the pain goes away?” My parents were on the phone, and I was in the hospital, still so consumed by the pain that I didn’t even care that I had just been informally diagnosed with cancer.
On the other hand, I can’t even imagine being a parent on the receiving end of that phone call.

What were the next steps after the lymphoma diagnosis?
The doctor explained that I would have to undergo a few more scans and that the mass in my chest needed to be biopsied.
It would confirm my diagnosis. From that point onward, I would meet my oncologist.
Getting re-staged to stage 4B Hodgkin’s lymphoma
The biopsy showed it was Hodgkin’s. When I met my oncologist in early February while I was still in the hospital, I was told that based on the CT scans and results of other tests performed, it appeared that I had stage 2B Hodgkin lymphoma. She sent me for a PET scan to confirm the staging.
When I was told it was stage 2, I remember thinking to myself, ‘There’s no way it’s not stage 4, not with the symptoms I have faced.’
I looked at my doctor and said, ‘Keep looking.’
We learned the results of my PET scan at my first treatment, which was when I saw my oncologist next. She went through all the details and said that my treatment plans changed slightly because my cancer was stage 4 cancer.
I remember thinking in my head, “Thank you for finding it.” I knew there was more than what met the eye. In fact, I knew it in 2017.
How did they describe the B part of the diagnosis?
For lymphoma, there’s a standard type and a B type, which is referred to as including unfavorable symptoms. That’s when you experience things like weight loss, 10% or more in 6 months, night sweats that are ongoing. That’s what sums up the B component of lymphoma.
How did it feel to finally have an answer?
It was a major relief to me at that time. With that said, I hadn’t actually processed what was going to happen next, so I was just glad to know that all my symptoms came with a reason, beyond what was being chalked up as IBS, scoliosis and psychological.
Preparing for Treatment
What do you remember from the biopsy?
A biopsy is when they make a tiny incision (that’s how mine was), and they take out a little piece of the mass that exists. For some people, they take out a lymph node and send it for pathology. That’s how they find out if it’s cancerous.
Describe the PET Scan
You go in, and they inject a dye with sugar in it. Essentially, the tumors that are inside of you will suck up that sugar. On the scan, it shows up. The machine looks similar to a CT scan. You go in, and similar to any other scan, you’re lying still for the duration of it.
I can’t tell you how long it was. I try not to remember that part so much with most of the tests. I truly can’t say I remember much about lying in the room for the PET scan. It wasn’t really relevant to me. It didn’t bother me. I just remember how it works.
How did your oncologist describe the treatment plan?
Chemotherapy treatments for 6 months, ABVD chemotherapy. I know for different staging, they do radiation therapy. For me, they didn’t consider that.
How did you break the news to your loved ones?
My parents found out during our phone call while I was in the hospital with an ER doctor, who delivered the news over that call. I told my closest friends over the course of the next several days, while I was in the hospital.
When you are ill and you have to deliver the news about it to those whom you love, you already know the pained responses that it will elicit. The common idea to look for solutions and ways to alleviate that pain only leads to a “no exit” road sign; you know that nothing in your power will fix it.
Delivering heartbreaking news to the people you love comes with knowing that the news is going to hurt them and that there is nothing you can do to relieve the pain that it inflicts.
It can feel like you are causing pain. It is important to try to remember you’re not. Sometimes you feel like you have to console the people around you, and you do. I know that exists for many cancer patients, because there’s nothing they can do to fix the problem.
What people really want to do is fix the problem. The truth is you can’t. You can just be honest.
»MORE: Breaking the news of a diagnosis to loved ones

How did you allow yourself to be supported?
I found it difficult to let myself be supported. I wanted to continue to be as independent as I had been. I was the person other people seemed to turn to.
It took a lot effort and consistency for several years, but I had my life together. I liked who I was. I often pushed the people I loved away from me during what felt to me like my weakness, because I didn’t want to disappoint them.
I knew that my weakness would be a place for some people to project their lives and insecurities. The idea of being undermined because I couldn’t be the friend I had always been, and because I finally cracked and couldn’t be the girl who had it together as I battled cancer, turned my stomach in knots.
The worst part was that it came when I was already beating myself up for what I couldn’t be during those months.
In the end, here’s the deal: if you have people around you who want to be present with you and care for you, let them.
If they undermine you later, they weren’t your friends to begin with. You’ll learn who they are very quickly in silence. Don’t assume everyone else around you is like that, or else you’ll isolate yourself from everything good.
I did that to myself during the 6 months I faced treatment. I was around people, but I didn’t let them in. Running was the only support I accepted, not wanting to be a burden on anyone else.
Looking back, I am pretty sure not taking for the first while added the burden that others felt. One of the biggest lessons you’ll learn from those who stick around through your worst, during the treatments and the several months which follow after them, is how to take.

If you are a giver, you know how to give. But to take, you have to trust the people who are giving to you. When you are battling cancer, you have this opportunity to learn to take, and also to learn who wants to give unconditionally. You learn who you are and who others are very quickly.
The only thing that the people who love you can do for you when they know they can’t fix cancer is show up and be there with you. You may feel like you can do it on your own, and maybe you can, but that’s not the point. Let them be with you.
Let people who care be there for you, because that is their ability to show you how much they love you, and it counts for them, too.
It takes a village of family and friends who love and support you — and strangers who have no idea who you are but inspire you from afar — to get through it.
Don’t try to brush past it. Allow it to sink in for other people, too. You go through your own grieving process, and more often than not, you start coping from the get-go.
Coping through a diagnosis and then a cancer battle feels similar to coping with a high-stress emotional event the night before a major exam. If you have an exam tomorrow and something hits the fan tonight, you’re going to tell yourself, “Okay, this just happened, but I need to be prepared for my exam so I can succeed, so I’m going to deal with this after the exam.”
Except when you’re coping with cancer, your exam isn’t a few hours long. It is 4, 6, 8 or many more months long, so you’re just coping all the way through it.
All of a sudden, when treatment finishes — if it does — you’re lucky enough to be left with the emotional burden from 4, 6, 8 or more months ago, which was suppressed during that time to simply get through it. It is a mean feat to face.
If there’s a bright side that exists, it is in our ability to learn how to take the pure care and deep love that others are so willing to give to us during the most difficult times in our lives.
It’s difficult because you have a sense of who you are and who you’ve always been. You can do what you want because you can, but when you’ve just been diagnosed or just started your treatments, you haven’t quite realized that in just a few months you might not be able to be the person who you have always known yourself as and who you have always been.
If you can grieve and come to accept that loss before you reach that boiling point, you’re remarkable. I couldn’t, and the pain weighed on me every day. Yet everybody is still in your camp.
Letting others support you during your greatest vulnerability should lead you to feel a sense of pride. You are special enough to those people that they want to be there through your worst.