LaSonya’s High-Grade Bladder Cancer Story
LaSonya D., Bladder Cancer, High-Grade
Symptom: Blood in urine
Treatments: BCG immunotherapy, surgery (cystectomy)
LaSonya’s High-Grade Bladder Cancer Story
LaSonya was diagnosed with high-grade bladder cancer. As a nurse practitioner, she used her experience to do her own research so that she knows that she’s getting the best care possible.
She shares the importance of listening to your body and advocating for yourself, seeking the care you want and deserve, and getting all the information you can to make the best decision for yourself.
The interview has been edited only for clarity. This is not medical advice. Please consult with your healthcare provider for treatment decisions.
- Name: LaSonya D.
- Diagnosis:
- High-grade bladder cancer
- Symptom:
- Blood in urine
- Treatment:
- BCG immunotherapy
- Cystectomy (bladder removal surgery)
Listen to your body. If you feel like something’s not right, it’s not right.
Pre-diagnosis
Introduction
I am a variety of things. I’m a black woman, but I’m also a mother [and] a wife. I am a professor of nursing. I am a nurse practitioner of both family and women’s health.
When did you start feeling that something wasn’t right?
I’m really in tune with my body. If something is off, I find out what’s going on right away. I don’t waste time trying to figure things out.
I had just recovered from an elective procedure and was getting ready to go back to work. One day, I noticed blood in my urine. It seemed like it was a lot of blood. I saw some blood clots and I was thinking, I know I’m not on my menstrual cycle. What is going on? Maybe it’s something from my surgical procedure. Although it was time for me to go back to work, [my surgery] had been a month prior.

I called my surgeon and he said, “It doesn’t seem like something related to your surgery, but we’ll go ahead and have you do a urinalysis and see if you have a urinary tract infection.” I did that [and] it came back negative for infection, but positive for blood.
He said, “You need to follow up with your primary doctor.” Fortunately, I used to work for my primary doctor so I know her well. I called her on her cell phone and she said, “Why don’t you go and do a culture? In the meantime, we need to do a CAT scan of your bladder.”
A few days later, I went in for a CAT scan. It came back [showing] I had a mass in my bladder.
Finding that I had a mass in my bladder was devastating news. I was really, really thrown back by it. I was like, ‘Could it be a mistake?’

When you found out there was a mass, what was your reaction?
Being a nurse practitioner, I knew what that meant. If one of my patients [had] blood in their urine, I would have done the same exact test that my primary doctor did. It could be a urinary tract infection. It could be kidney stones. Worst-case scenario is bladder cancer.
The way I approach my patients is: Tell me why it’s not bladder cancer, like the worst thing. When somebody has a headache, why isn’t it a brain tumor? I was like, “Why is this not bladder cancer?” I would have done the same thing.
Finding that I had a mass in my bladder was devastating news. How did I get this? No one in my family, on either side, has a history of cancer. How could this be? I don’t even know one black person that has this type of cancer. I was really, really thrown back by it. I was like, “Could it be a mistake? It could be a cyst. It could be this.”
The next step was to see a urologist.
The doctor that I currently work with had a good friend that was the head urologist in [the] healthcare system we both work for. This is in January 2021 so we’re in the midst of COVID — a lot of delays trying to get surgeries and procedures done. She called him up and said, “My nurse practitioner [has] this going on. Could you please see her?” Fortunately, I was able to get an appointment the following week.
I felt so defeated and deflated. I just could not believe that this was happening to me.
Diagnosis
How was it hearing the words come out of his mouth?
I was already prepping myself mentally, but it was still devastating. I was a nervous wreck. I remember having to take off work because my blood pressure [was] through the roof. I felt so defeated and deflated. I just could not believe that this was happening to me. It took me a week or two to get myself together mentally for what was next.
Next, they needed to biopsy, resect it, and see what stage of cancer it was. I started doing a lot of reading. My biggest concern was: Is this muscle invasive? Because if it is, that means that I’m going to have to have my bladder removed, chemo, and all this stuff is going to happen really fast.
My first husband passed away [from] lymphoma. My older two kids are still in [a] deep stage of grief. For them to find out that their mom has cancer was really tough.
Being the glue of the family
My first husband passed away [from] lymphoma. At that time, it was about five years prior. My older two kids are still in [a] deep stage of grief after losing their father at 47 years old. He went downhill in a matter of three years. For them to find out that their mom has cancer was really tough.
My youngest son was away at school. He’s a dancer. He’s at the University of North Carolina School of the Arts High School. We didn’t want to tell him until he came home for summer break. There was no reason to let him know right away other than to get him all upset and worried.
It was rough, thinking about your own morbidity and your potential mortality, especially when you’re thinking about cancer.

I’m a very, very spiritual person. I’m a Christian and I very much lean on my faith, which is another thing that helped me get through this. But, at the same time, my grandmother used to always say, ‘The Lord helps those who help themselves.’

Seeking help from a therapist
I knew right away that this was going to be very stressful, not just for me but for my family. In order for me to get through this, I was going to need help.
I contacted [a friend from church] and asked if she would take me on as a client and she agreed. Right away, I started meeting with her once a week. Our meetings continued through my first treatment, from February through May. I would meet with her on a regular basis, which was so helpful for me.
A lot of times people think that you have to take on everything yourself. Especially [in] my culture, mental health is very taboo. People take it as a weakness when you need to seek out help mentally. You always hear people say, “Be strong. Suck it up. You can do this. Don’t be weak-minded.” We are human beings. We are not robots and machines. We have feelings. We have difficulty.
Or they’ll say, “Pray about it. Give it to God.” I’m a very, very spiritual person. I’m a Christian and I very much lean on my faith, which is another thing that helped me get through this. But, at the same time, my grandmother used to always say, “The Lord helps those who help themselves.” It’s important for us to help ourselves. Part of that was interacting with a therapist that could help me — someone that I could trust and someone outside of my house, my family, and my life.
It was enough for me to talk to my husband but there were some things that I was going through that I didn’t necessarily want to tell him and burden him with. He had his own burdens of worrying about my mortality or my morbidity. I wanted to be able to freely talk without having to worry about someone else’s feelings about what I was going through and it was very helpful.
I never have been one to put all my trust in another human being so I felt like I needed to do my own research and have my own questions ready so that I know that I’m getting the best care possible.
Figuring out the next steps
The first thing I did was look for a reputable bladder cancer organization. You can find anything on the Internet — some of it is true, some of it is false. You can find people that will sell you snake oil and a bucket of sand. At the same time, you can find medically-sound information.
Because I am a scholar and also a clinician, the first thing I did was pull research articles and guidelines of practice because I wanted to know what to expect. I wanted to know if whoever I was going to see [was] following the correct guidelines to take care of me or not. I never have been one to put all my trust in another human being so I felt like I needed to do my own research and have my own questions ready so that I know that I’m getting the best care possible.
The experience I had with urologists made it even clearer to me that my approach is the best approach for me. Despite the fact that I was a clinician — I actually worked in the same healthcare organization that he worked in — he did not treat me well as a patient. And thankfully, because I’m a clinician, I was able to identify that right away. But when you’re talking about lay people going to seek care, go with your gut.
If you feel like something is not quite right, get a second opinion. You’re entitled to a second opinion. Some insurance will even pay for a third opinion. Do not feel like you’re stuck with that person.

Go with your gut. If you feel like something is not quite right, get a second opinion.
Appointment with the urologist
The urologist talked to us about the procedure. He scoped my bladder and said matter of factly, “Oh, it’s bladder cancer. It’s definitely bladder cancer. But I think it’s really superficial. It’s probably not a big deal. With COVID, it’s hard to get an OR so we can schedule this out.” I said, “No. If you can’t do it, I can find a surgeon that can do it. I have very good insurance. I have a PPO. I can go anywhere I need to go. I have something growing inside of me that doesn’t belong here and I want it out.” So he was like, “Okay, I’ll go ahead and do it.”
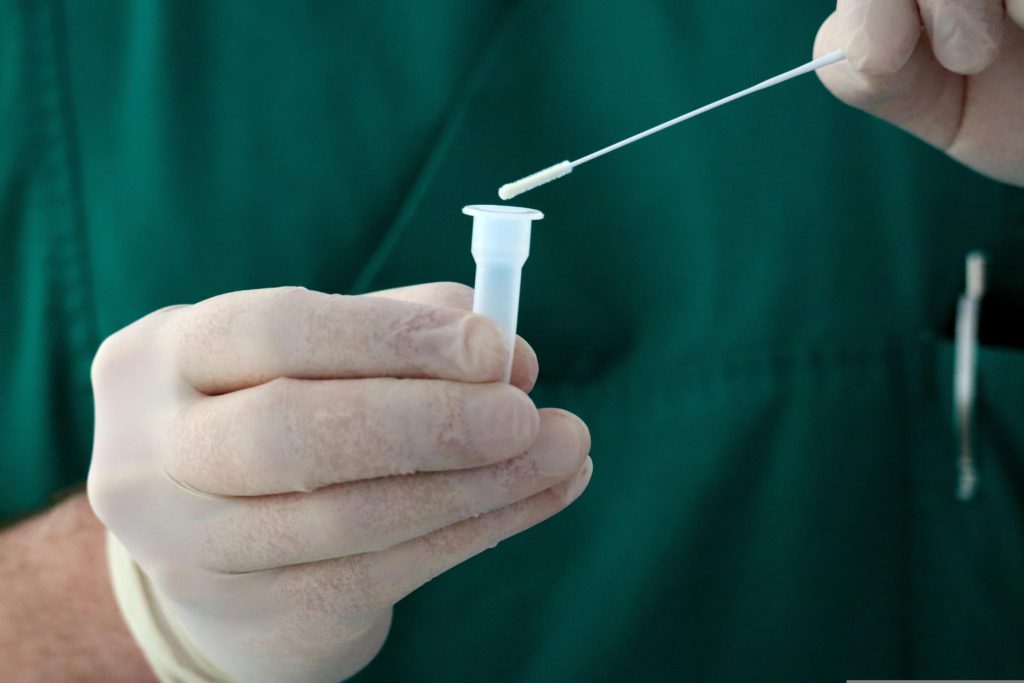
He had someone come up to give me a COVID test because you had to have a COVID test before you could schedule your surgery. He said I can have my surgery in a week. The lady came up and did my COVID test. I didn’t notice at the time but when I think back, I didn’t see her label my specimen. Long story short, the COVID test came back positive.
How do I have COVID? I’ve been home for four weeks because I had that surgical procedure. My husband’s working from home and we’re the only ones here. We’re very, very careful and cautious. For a whole year, I’ve been working in the field, in the clinic, with patients, some with COVID, but I hadn’t had COVID. I was like, “Something’s wrong with this.”
I called my clinic and had them do another COVID test. That test came back negative. I called them and said, “I had a false positive test. This new test is negative. I do not have COVID.” They said, “Oh, well, he’s going on vacation.”
He was gone on vacation. I kept calling and advocating for myself to get on the schedule so I was able to get on the schedule for the following week. Three weeks after diagnosis, I was able to have my surgery for the resection.
During the time that I was waiting to have my surgery, I had questions for this doctor so I [sent an] inter-office message.
I checked into the hospital [on] the day of my surgery. During that time, you couldn’t have visitors so my husband couldn’t go with me to pre-op. I had to go by myself, which was very nerve-wracking. I was nervous. I didn’t know what’s going to happen.
If you’ve ever been into pre-op, there’s just beds and curtains between them so you’re not in a room by yourself. You’re in this big room. I go in pre-op. They prep me. They start your IV, get your history, [have] you sign your consent, and all those things.
He comes in before surgery and says, “Okay, we’re ready to do your surgery. I can tell you’re a very highly anxious person.” I’m thinking, Should I say what I really want to say? Or should I just not say what I really want to say? This man is getting ready to operate on me. I’m going to be asleep. He’s going to have instruments inside of me so I’m not going to say anything to put myself at any risk. So I said, “Yes, I am.” Whatever it takes for you to feel good about yourself to do what you need to do, that was my thought process. And he goes, “Well, you inter-officed me, but please don’t do that again. Do not inter-office me. If you’re going to email me, email me through the patient portal.”
I’m listening to him and thinking, We are in pre-op. You’re getting ready to resect my tumor to find out if I have cancer, if it’s superficial like you think it is. You don’t know everything. How can you tell me that this is not invasive cancer by looking at it with your eyeballs? I was like, “No, I’m not trusting that you saying superficial is enough and I want it out now.” I’m sitting here thinking, Okay, now you’re going to chastise me in the pre-op area for something that we could talk about at another time. That email [was] sent probably a week or two before so this is not urgent. You’re on vacation the whole week before so there was no reason for us to talk about that right now.
We had the surgery. Everything went well. Then he says, “It’s going to pathology and then we’ll find out what the situation is.” I said, “Okay.”

Feeling like your doctor is talking down to you
He did not see me as a colleague the way he was chastising me, in front of my colleagues, fellow nurses, and other patients. It could have been one of my patients in there with me. We’re all in the same healthcare system. He had no consideration of that. The little respect that I had left for him, I actually lost right in there.
The first thing I thought: I will never, ever in a million years refer any patients to this person. Congratulations. You will be a star in my book and the chapter is probably going to be, “Do Better,” because it was uncalled for.
If you have to drive an hour and a half or two hours to get the care that you deserve, you need to do that. How far would you drive for life?

Treatment
Getting the care you want
When I got home, I talked with my husband. We decided that once I got a definitive diagnosis, I was going to transfer my care to City of Hope. I wanted to do that because my great aunt [who] had melanoma went to City of Hope and they gave her excellent care. I was like, “We have the insurance so we can do it so let’s just do it.”
From where we live, City of Hope is about an hour and a half [away]. My husband just said, “It doesn’t matter how far it is. I’m going to take you wherever you need to go.” And for me, that’s something I can’t express more powerfully.
If you have to drive an hour and a half or two hours to get the care that you deserve, you need to do that. I tried to get my ex-husband to transfer his care to City of Hope. I tried for almost a year. Finally, when he decided that he was ready, he could not transfer. He was too ill.
City of Hope [doesn’t] have an ER. It’s a cancer hospital but you have to enter as an outpatient. By the time he decided that he wanted to go, he was an inpatient at UCLA. He could not leave the hospital. He was so ill. He was there for a month. He came home for one night and was back at the hospital the next day. Never could get him strong enough so that he could be seen there.
I kept telling him they’re doing a special trial for his type of cancer. He really needs to try to get there. But he never did. I think the first thing that he said was, “It’s so far.” It’s only an hour and a half away. How far would you drive for life? And life more abundantly. How far actually would you go?
Getting the results from pathology
We went back to the doctor and the doctor says, “I’m so sorry. I thought that this was superficial but you have high-grade bladder cancer. Even though we removed the tumor, these types of cancers have a very, very high likelihood of returning.”
The good news was that it hasn’t gotten to the muscle, but it is in the lamina propria, which is the lining inside of the bladder and the bladder wall. He said that they took an extra sample just to make sure that they were not missing anything. It was deeper than they thought it was, but it looks like there was no muscle in the tissue.
When he told us, my husband and I began to celebrate. We were happy. We were thanking God because we knew that if it was in the muscle, that [meant] chemotherapy, bladder removal — all that was going to happen, that was the next step. But if it was not in the muscle, I can at least try another treatment, which would have been BCG immunotherapy installations into my bladder over a series of time and then maintenance for three years. And if no recurrence of tumor, then I may be cured at that point.
We started celebrating and he said, “No! No! No! This isn’t anything to get excited about. This is serious. It’s high-grade cancer.” I was telling him, “Excuse me. This is something to celebrate because today, I get to keep my bladder. I’m not worried about what’s going to happen in a year, two years, or three years down the line. But this day, I get to keep my bladder and that is a blessing.”

Then he was like, “I really want you to go and have a second opinion with my colleague at USC.” I was thinking, Excuse me. The way you have treated me, there’s no way that I will ever go to anybody associated with you because they will likely be just like you and I’m not doing it. I tell him, “No, thank you. We’re going to City of Hope.” And he said, “Why do you want to go to City of Hope? It’s so far. Is there a particular reason?” I said, “Because that’s where we want to go.”
My husband interjected and said, “I will take her wherever she needs to go. If we have to get on an airplane, we will be doing that.” And I was thinking, Yes, we are those black people, not the ones that you think we are. I’m sitting here going, How dare he? The audacity to try to discourage me from going to a cancer treatment center, [an] internationally-recognized cancer treatment center, because of the distance.
I’m not worried about what’s going to happen in a year, two years, or three years down the line. But this day, I get to keep my bladder and that is a blessing.
He was saying, “We could do the BCG, which is the immunotherapy here, but there is a BCG shortage.” And this is true. There’s a national shortage of BCG because only one company makes it and I knew that. I also knew if you’re in a cancer treatment center, because of the other drugs that the hospital uses, they’re more likely going to make sure that they give them what they need first.
I felt like I was going to get a better chance of getting my BCG and getting it on time if I went there as well. We don’t think about these things as lay people, but this is something that I was able to think about and pre-plan. He probably wasn’t too thrilled [about] that. I just said, “Thank you very much. I appreciate all that you have done. Goodbye.”

Dealing with preconceived notions in healthcare
He had a picture in his mind of who I was and what my life was like. He already had his own stereotypical thoughts about who I was. Because if he didn’t, he wouldn’t have treated me that way. Not because I was his colleague, but because I was his patient. He wasn’t seeing me as a colleague, even though I was. He was seeing me as a black patient.
I don’t really know. Maybe he treats all his patients that way, but being a black woman and seeing the health disparities that we have in particular compared to other groups, I thought that he felt that he had the right to treat me the way that he did.
Why wouldn’t he say, “Well, you know, City of Hope’s an hour and a half away. Is that going to be a problem for you?” Why not say that? No, he just assumed that we couldn’t do what we needed to do or we wanted to do as far as my care went. My husband should have never had to interject and tell him, “If she needed to get on an airplane to go somewhere to get care, then I’m going to do that for her.” We shouldn’t have even had to have that conversation.
I had an aortic aneurysm. I had heart surgery at 39 years old. My doctor, my cardiologist, he is a man of color. He is Indian. When I first went to him, was diagnosed, and knew that I had to have open heart surgery, the first thing he said [was], “Now I can do this surgery right here. But because of your age, I want to send you to San Francisco. I don’t know if you know this basketball player.” He was telling me about a basketball player who had the same thing, an aneurysm. And he said, “He plays with a vest on. He had his surgery in San Francisco and they did a great job. And I think because of your age, I really want you to go there.”
He never assumed that I wouldn’t be able to go there. He never assumed that we couldn’t afford to go there. He didn’t have any assumptions. He said, “In my personal opinion, you would receive the best care here. And this is where I would like for you to go if you could.” And that’s the approach that the other doctor should have taken. It’s only an hour and a half away. How far would you drive for the best chances? The latest equipment [and] doctors that are doing research actively on your problem. Why wouldn’t you?
He said, “You will never come back here.” I said, “Touché. I’m not coming back here.” He did exactly what we needed him to do — make the initial diagnosis and that was it.
I was looking for a doctor that looked like me because I felt like I could trust a doctor that looked like me.
Transferring care to City of Hope
It was so easy. The first thing I did was pull up their different offices. Come to find out, they have clinics all over. They have offices all over California, not just in Duarte. The closest to us that has urology was in Santa Clarita. From our house, it probably takes us 45 to 50 minutes to get there. If anything needs to be done, like hospitalizations, then you go to the other place. But you can have your regular visits, including the treatment for cancer, right there in that office.
I looked at all the doctors. I was even willing to go to Duarte if I had to. I was looking for a doctor that looked like me because I felt like I could trust a doctor that looked like me. Fortunately, I found one.
When I’m taking care of patients, I look at them holistically. For example, in my clinic, probably 95% of my patients are Latinx. Most of them [are] farmworker families. Majority do not speak any English at all. I speak a little bit of Spanish, but I try to find out everything I can about the culture. I want to learn as much as I can learn about the culture because those are my patients. Those are the people that I’m seeing. When I’m taking care of them, I’m not just taking care of what’s right in front of me. I’m looking at them holistically as people, as a culture, [and] as a community. And that’s what I felt like I needed in my health care.
I need someone who knows the culture so I don’t have to explain every little thing to them and they know how to approach me as a person probably because they have some shared experiences with me. Unfortunately, the doctor I selected was not a urologist. Urogynecologist but not a uro-oncologist, which is what I needed for my problem so I had to pick someone else. And I did and it worked out really well for me.

Discussing treatment with the new team
Even if I were to stay where I was, there should have been a second resection. What helped me is their bladder cancer advocacy. There’s an organization (the Bladder Cancer Action Network) that gives patients tons of information. It’s like the American Cancer Society for bladder cancer. I was able to pull articles, look at the actual standards of care, [and] the procedure so I knew what was supposed to happen.
If it comes back negative for muscle invasion the second time, after your bladder recovers [in] about four to six weeks, they start you on immunotherapy, which is installation of the treatment into the bladder. I had to do that for six weeks.
The new doctor did the resection. I really liked her a lot. Liked her personality. She was very positive, which is what we were looking for. The resection turned out really well. Then we were going to start the BCG.
BCG immunotherapy for bladder cancer
My path was a little bit different. They did the first six weeks of BCG. During that time, I had one bladder infection that delayed treatment for a week because I had to take antibiotics then I had to go back and finish. At the end of it, they wait eight weeks and then they scope you.
It’s an infusion directly in your bladder. You have to hold it in your bladder for two hours then you can pee it out. When you start peeing it out, you have to put bleach in the toilet and be careful that nobody else uses the toilet.
The BCG was better than chemo, but it was hectic.
Side effects from BCG immunotherapy
The first day, I would be fine. Second day, I would have joint pain, flu-like symptoms, [and] fatigue. I might have pain with urination [and] bladder spasms. The more treatments I had, the more irritated and the more irritable it became.
The BCG was better than chemo, but it was hectic. With the burning with urination, it didn’t matter what they gave you, it just was not going to do it. It might take the edge off, but that was pretty much it. It’s like making your bladder raw on the inside, too, to make the environment not conducive for the tumor to grow.
Maintenance therapy for bladder cancer
The following month was my first maintenance dose of BCG, which was for three weeks — a lot better than the six weeks. Then eight weeks later, I would be scoped.
On the eighth-week scope, I had no new tumors that they could see, but they saw a bumpy area. She wanted to watch it. At that point, you would be having maintenance BCG immunotherapy every three months for whatever the prescribed time was going to be. It could be two years, three years, [or] five years. Maybe two years and then [on] year three, you do it every six months. It just depends on how well your progress is going.
My bladder is actively trying to kill me. It’s my bladder or me. What’s it going to be? I decided I’d rather it be my bladder to go.
Bladder removal surgery
New development leading to bladder removal surgery
When I had my second scope after the three-week BCG maintenance, that’s when my treatment took a different turn.
When they went in to scope my bladder again, I didn’t have any tumors but that bumpy area had gotten bigger. The doctor said, “I want to take it out.” And I said, “I want you to take it out.” I was so happy that she wanted to do the procedure.
She went in, resectioned it, pulled it, took it out, [and] sent it to pathology. When she was in there, she found another small tumor that wasn’t even detected on the scope so she took that out, too, and sent that to pathology.
That area that was flat and bumpy was the same cancer that I originally had. It just wasn’t growing in the bladder. It was growing down so it had not reached the muscle yet, thank God. It had gotten to that layer, but it hadn’t broken through to the muscle wall. Again, that makes the difference between chemotherapy [and] something else.
She also found another type of bladder cancer: carcinoma in situ. I had already done some research and I knew that most people who have that, it just comes back. It’ll be one now. Next time, it’ll be three. Next time, it’ll be five. All roads eventually lead to bladder removal for most people.
Every time, in all these treatments, you’re rolling the dice that it’s going to get to the muscle. My bladder is actively trying to kill me. It’s my bladder or me. What’s it going to be? I decided I’d rather it be my bladder to go.

I’m going to stay here. I’m determined to be here. If I go ahead and do the surgery, I have choices [regarding] the outcome. If you wait too long, it can get into the bladder wall [or] outside of the bladder wall. The wall of the bladder is very thin. It sits right on top of the uterus. Once it gets out, it goes [quickly].
You’re taking chances. And I’ve never been one to really take a lot of chances, especially with my life. I know my kids need me. I know my husband needs me. I have a lot of responsibility and I really want to be here.
At that point, I made the active decision to have my bladder removed. I talked to my doctor and when she gave me the final pathology, I said, “I really think that I want to have my bladder out.” And she goes, “You know, I was going to tell you, you could do inter-bladder chemotherapy because it’s not in the muscle. We can put the chemo in your bladder but [it] may not work. It probably won’t, long-term. If it were me, I would do the same thing.”
At that particular point, that was the reassurance that I needed. But I already made up my mind that I was going to do it.
I’ve never been one to really take a lot of chances, especially with my life. At that point, I made the active decision to have my bladder removed.